Introduction
Some patients with dizziness show abnormal findings in otolith function tests despite normal semicircular canal (SCC) function [
1]. The dizziness in such cases is presumed to be due to an otolith organ-specific (isolated) disorder. The saccule and utricle are sensors of linear acceleration. Therefore, isolated otolith dysfunction (iOD) [
2] may produce symptoms such as tilting, translational sensations in the roll plane [
2], translational sensations in the pitch plane [
3], or drop attacks. It has been reported that patients with otolith functionrelated symptoms have a greater chance of positive findings in cervical vestibular evoked myogenic potential (cVEMP) and ocular vestibular evoked myogenic potential (oVEMP) (symptom-driven approach) [
4]. It has also been reported that patients with abnormal otolith function lab findings have a greater likelihood of swaying or rocking type dizziness (lab finding-driven approach) [
5]. However, there is no consensus on symptom definition and diagnostic criteria for otolith dysfunction. Furthermore, there is still a lack of consensus and standardization with regard to the test battery to be used for assessment of otolith function [
6]. Therefore, it is necessary to determine a set of diagnostic criteria for iOD with a structured definition based on the symptoms and lab findings.
Several different terms have been used to indicate iOD by different researchers. For example, some authors used the term ŌĆ£idiopathic otolithic vertigo (IOV)ŌĆØ [
2], defined as 1) episodic lateral tilting or translational sensations, or 2) episodic anteroposterior tilting or translational sensations, or 3) episodic up-down translational sensations. Others have introduced the term ŌĆ£otolith organ-specific vestibular dysfunction (OSVD)ŌĆØ [
1], defined as abnormal cVEMP responses to airconducted sound and/or oVEMP responses to bone-conducted vibration in the presence of normal caloric responses and normal video head impulse test (vHIT) recordings in each SCC plane. Isolated utricular dysfunction (iUD) has also been defined as the presence of a unilateral oVEMP abnormality and normal caloric responses [
5]. Although the definitions are slightly different, terms such as IOV, OSVD, and iUD are all aimed at classifying a specific group of patients with abnormal otolith organ function and normal SCC function. In most of the studies mentioned above, a normal caloric response was a prerequisite to guarantee normal SCC function [
1,
5,
7]. However, the false negative outcome of the caloric test in some patients may make this classification obscure. Some patients classified as OSVD or iUD in previous reports may not have had true iOD. It is possible that a significant proportion of patients in this group also had SCC dysfunction, but the caloric test results were normal due to false negative error. For example, the most common symptom of OSVD was rotatory vertigo [
1]. As physiologically rotatory vertigo is attributable to dysfunction of the SCC, we believe that the patients in this previous study did not represent true iOD. To overcome such problems, we propose that lab findings as well as symptoms should be taken into consideration in the diagnostic criteria of iOD.
This study was performed to classify iOD patients into two groups: an iOD group proven by lab findings (caloric and otolith function tests) without iOD symptoms (lab-based iOD group) and an iOD group proven by lab findings with accompanying iOD symptoms (lab- & Sx-based iOD group). We hypothesized that the clinical presentation of these two groups would be different because of differences in the true extent of the pathology in the inner ear. Despite the normal caloric response, both the SCC and otolith organs may be compromised in the lab-based iOD group, while the SCC is preserved and only the otolith organs are compromised in the lab- & Sxbased iOD group. We believe this study will help us understand a novel disease entity that has not been fully recognized in the past and understand the underlying mechanism of dizziness in some patients who cannot be fully explained by the classical vestibular function tests (VFT) (caloric test and/or rotation chair test).
Results
The demographics of the lab- & Sx-based iOD group and the lab-based iOD group are shown in
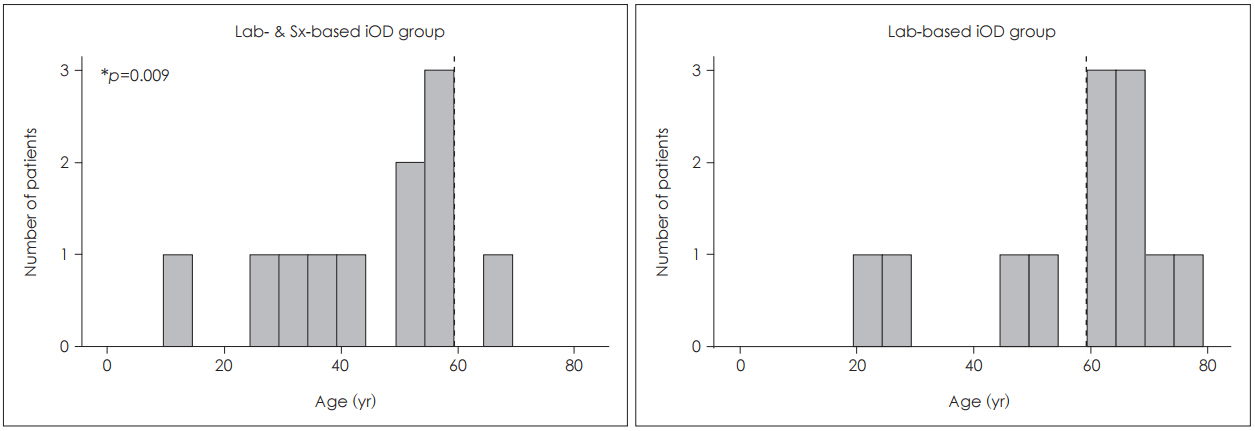
Table 1. The lab-based iOD group was approximately 15 years older than the lab- & Sx-based iOD group. The majority (66.7%) of patients in the lab-based iOD group were over 60 years old, while only one patient (9.1%) was over 60 in the lab- & Sx-based iOD group (
p=0.009) (
Fig. 1). There were no significant differences in gender ratio, frequency of vertigo attacks, duration of illness, or severity of dizziness NRS score between the two groups. All patients in the lab-based iOD group had spinning vertigo as their chief symptom, while all patients in the lab- & Sx-based iOD group had otolith organ-related vertigo (
p<0.001). Patients in the lab- & Sx-based iOD group described their symptoms as a horizontal floating sensation (n=7), flipping upside down (n=2), lateral translation (n=1), or up-down vibration (n=1). The utricle was the most frequently involved otolith organ (75.0-81.8%). Utricle involvement without saccular involvement was found in 50.0-54.5% of cases, while both the utricle and saccule were involved in 25.0-27.3% of the patients. There was no significant difference between the two groups in terms of extent of involvement.
Clinical diagnosis was idiopathic in 81.8% of cases in the lab- & Sx-based iOD group (
Table 2). That is, taking the symptoms and VFT findings together, the diagnosis did not correspond to any currently known vestibular disorder. Accordingly, the final diagnosis was idiopathic iOD. The clinical diagnosis was idiopathic iOD in only 16.7% of cases in the lab-based iOD group, which was a significantly lower incidence than that in the lab- & Sx-based iOD group (
p=0.003). The most common combined vestibular disorder accompanying iOD consisted of benign paroxysmal positional vertigo (BPPV) and M├®ni├©reŌĆÖs disease (MD).
The vHIT gain was normal in both ears in all subjects except in one ear of one subject in the lab-based iOD group (left horizontal canal gain was 0.7 in this subject). The gain was normal in all subjects in the lab- & Sx-based iOD group. Catchup saccades were found in 54.5% of patients in the lab-based iOD group. No catch-up saccades were detected in the lab- & Sx-based iOD group. The detection rate of catch-up saccades was significantly higher in the lab-based iOD group than the lab- & Sx-based iOD group (
p=0.012) (
Table 3).
More patients in the lab-based iOD group showed abnormal sway (72.8%) during mCTSIB compared to the lab- & Sx-based iOD group (45.5%). In particular, the EC foam condition (the most sensitive condition for detecting vestibular dysfunction) was abnormal in 45.5% of patients in the lab-based iOD group. Although higher than that of the lab- & Sx-based iOD group (27.3%), the difference was not statistically significant (
Table 3).
Discussion
The imperfect sensitivity and specificity of the caloric test can be a critical problem when defining iOD. The general definition of iOD is ŌĆ£abnormal function of the otolith organs despite the normal function of the semicircular canals.ŌĆØ In most studies reported to date, the caloric test was used as the gold standard to confirm normal function of the SCC [
1-
3,
7,
12,
19]. The validity of this definition is dependent on the sensitivity and specificity of the caloric test [
20]. However, the caloric test cannot be used to evaluate the superior and posterior canal function. It is also limited by the fact that caloric irrigation presents a low-frequency stimulus to the labyrinth [
20]. The sensitivity was evaluated according to the time delay from onset of vestibular neuritis, and was shown to be 100% up to 2 weeks, 80-85% up to 1 month, 75% at 3-6 months, and 65% at 12 months [
21]. That is, symmetric caloric responses did not exclude the possibility of canal dysfunction a few months after the onset of vestibulopathy [
20]. Considering the possibility of false negative results in the caloric test, it can be assumed that several months after onset of vertigo some subjects will be misdiagnosed as iOD despite SCC involvement. That is, a significant proportion of subjects in the lab-based iOD group may actually not have represented true iOD. The identification of vHIT catch-up saccades in more than half of the patients in the lab-based iOD group may support this hypothesis.
There are two possible interpretations for the vestibular disorders accompanying iOD, i.e., the accompanying vestibular disorder may have a causal relationship with iOD, or may simply be a bystander that is not directly related to iOD. The most common accompanying vestibular disorder was BPPV in this study, as also reported by other authors [
1]. Utricular dysfunction has been suggested as a possible mechanism of BPPV [
7]. For example, it has been reported that patients with BPPV have a tendency to show abnormal oVEMPs more frequently than cVEMPs [
22]. We also found that BPPV was more frequently accompanied by utricular dysfunction [oVEMP or SVV abnormality, 5/7 patients (71.4%)] than saccular dysfunction [cVEMP abnormality, 2/7 patients (28.6%)]. Considering the anatomy of the inner ear, it is strongly suggested that the detached otolith debris of BPPV originates from the utricle. In this sense, iOD (more specifically utricular dysfunction) may be the cause of detached otolith debris and, consequently, the cause of BPPV. On the other hand, BPPV and iOD may have no causal relationship in some patients. Incidental comorbidity is plausible considering the high prevalence of BPPV. For example, in our patients, BPPV did not occur at the same time point as iOD. Considering the time difference between the onset of BPPV and the onset of iOD symptoms, it is unlikely that iOD was a direct cause of BPPV. MD was also a frequent vestibular disorder accompanying iOD in this study and in that reported by Iwasaki, et al. [
7]. Endolymphatic hydrops in the saccule and utricle may explain the abnormal findings of cVEMP and oVEMP. That is, in some cases, MD may be a cause of otolith dysfunction. Approximately half of all MD patients are thought to show abnormal cVEMPs and/or oVEMPs during the quiescent period [
7]. In addition, a human temporal bone study showed endolymphatic hydrops in the saccule and utricle [
23]. In our case series, it was not clear whether the accompanying vestibular disorder (BPPV or MD) was the cause of iOD or merely a bystander. However, as there can be a causal relationship between the accompanying vestibular disorder and otolith dysfunction, we may not be able to classify these patients as idiopathic iOD.
One problem in classifying lab- & Sx-based iOD is that it is still not clear which symptoms are characteristic of otolith dysfunction. Vestibular symptoms caused by otolith dysfunction have traditionally been suggested as a tilting sensation, a sense of moving to and fro, lateropulsion, or feelings of falling [
7]. Furthermore, swaying, rocking [
12], tilting, a pulling sensation in the anteroposterior direction, and a somatosensory illusion of walking on pillows or on uneven ground were suggested to originate from otolith organ dysfunction [
19]. Recurrent drop attacks also represent a well-known symptom characteristic of otolith organ dysfunction [
19]. Previous studies revealed cVEMP abnormalities in MD patients with vestibular drop attacks [
1]. Human histopathological studies have found damaged otolithic membranes in the utricle in patients who have had multiple episodes of TumarkinŌĆÖs drop attacks [
24,
25]. However, our cohort included no iOD patients with repeated drop attacks. Fujimoto, et al. [
1] reported that only one of 28 iOD patients experienced repeated drop attacks. It seems that intuitive pathophysiological assumptions about iOD are not always consistent with the actual clinical symptoms. That is, it may be difficult to define otolith-specific symptoms. However, to classify the lab- & Sx-based iOD correctly, spinning vertigo should be strictly excluded from the otolith-specific symptoms.
The observations outlined above raise questions about how the utricle and/or saccule can become compromised while other parts of the vestibule, especially the SCCs, remain intact. The pathophysiology of iOD has not been elucidated [
2]. Based on the differential blood supply and innervation patterns, it is possible for a vestibular disorder to involve only a portion of the peripheral vestibular apparatus [
26]. One hypothesis is that viral activation can involve a selected portion of the inner ear or selective segment of the vestibular nerve without involving other parts of the inner ear. It has been reported that vestibular neuritis does not necessarily affect the complete labyrinth, but can involve only partial loss of vestibular function [
27]. The patients with lab- and Sx-based iOD in this study may correspond to this observation, indicating that even more specific lesions of the otolith organs can occur. With regard to other possibilities, Schuknecht [
28] reported experimental degeneration of otolith membrane by cutting the anterior vestibular artery. Selective hydrops of the utricle and/or saccule can also be responsible for iOD. It has been reported that the otolith organs develop endolymphatic hydrops more frequently than the SCCs [
23]. In addition, a mathematical model showed that the SCCs are most resistant to hydropic expansion, while the saccule is most vulnerable [
29]. Although the precise pathophysiology of iOD is not clear, previous observations indicated that selective vestibulopathy of the utricle and/or saccule may be possible.
Based on the findings of this and other studies, we propose structured diagnostic criteria for iOD (
Table 4) consisting of definite iOD and probable iOD. Probable iOD may be further subclassified into Sx-based iOD (as in IOV) and labbased iOD (as in OSVD) to indicate the rationale for making a diagnosis of iOD. Definite iOD requires both lab findings and symptom characteristics consistent with iOD (lab- & Sxbased iOD). Lab- & Sx-based iOD (definite iOD) may be considered as the only pure or true iOD. Probable iOD allows for some degree of uncertainty. For example, Sx-based iOD may be debated because there is currently no consensus on which symptoms are pathognomonic for otolith dysfunction. The lab-based iOD may also be classified as probable iOD and not definite iOD because, in some cases, vestibulopathy involving the SCC may be misclassified into this group due to the insensitive caloric test outcome. The definition of OSVD in the study by Fujimoto, et al. [
1] was similar to the lab-based iOD group in the present study. As shown in
Table 4, there were many similarities between OSVD and the lab-based iOD group. Age, gender, prevalence of spinning vertigo as symptoms, inner ear organ involvement, and accompanying vestibular disorders were similar between the two studies. These clinical similarities were the basis of classifying lab-based iOD into one category. Meanwhile, the clinical presentations were quite different when compared to definite iOD. Therefore, we should differentiate probable iOD from definite iOD. If the etiology of definite iOD is not clear, it may be indicated as ŌĆ£idiopathic definite iOD.ŌĆØ If an accompanying vestibular disorder, such as MD, is presumed to be the cause of iOD, it may be referred to as ŌĆ£secondary definite iOD.ŌĆØ We hope that the new definition of definite iOD will help researchers to identify patients who are more likely to be true cases of iOD, and facilitate comparisons of results between different studies.
In conclusion, we screened for patients who had vestibular symptoms and showed abnormal cVEMP, oVEMP, or SVV without canal paresis. Dizziness can be attributed to an otolith organ-specific (isolated) disorder, and iOD may be a distinct cause of dizziness in these cases. Although the lab findings were similar in iOD patients, patients with otolith-specific symptoms (lab- & Sx-based iOD group) and without otolithspecific symptoms (lab-based iOD group) may be different. We found clear differences between the lab-based iOD group and the lab- & Sx-based iOD group in terms of subjective dizziness sensation, age, accompanying vestibular disorder, and detection rate of catch-up saccade during vHIT. Based on these results and those of previous studies, we propose structured diagnostic criteria for iOD consisting of definite iOD and probable iOD. Definite iOD requires both lab findings and symptom characteristics consistent with iOD (lab- and Sxbased iOD). Strictly speaking, lab- and Sx-based iOD may be considered as the only pure or true iOD. Probable iOD allows for some uncertainties, such as inconsistent symptoms or inconsistent lab findings. We hope that the new definition of definite iOD will help researchers to identify patients who are more likely to have true iOD, and facilitate comparisons of results between different studies.